A gene called FOXJ1 may drive resistance to taxane chemotherapy during treatment for advanced prostate cancer, according to a new study led by investigators at Weill Cornell Medicine and Beth Israel Deaconess Medical Center. The findings provide important new insight into why patients with metastatic disease often stop responding to a key class of life-prolonging chemotherapy drugs after initially benefiting. Given that taxanes remain the only chemotherapy agents with demonstrated survival benefit in advanced prostate cancer, understanding how and why resistance develops is an urgent need for patients.
The study, published Feb. 14 in Nature Communications, suggests that doctors may be able to measure FOXJ1 gene activity in tumors to predict which patients could develop drug resistance and move directly to alternative therapies, avoiding unnecessary toxicity.
“This is a previously unrecognized role for the FOXJ1 transcription factor, and it could serve as a potential biomarker to help us identify patients who are more likely to benefit from these types of treatments,” said Dr. Paraskevi Giannakakou, professor of pharmacology in medicine and director of laboratory research in the Division of Hematology and Medical Oncology. “In addition, the research opens the door to developing future therapies that could block this resistance pathway and restore drug effectiveness.”
Surprising New Role for FOXJ1
The Beth Israel Deaconess research team created mouse models of prostate cancer that had become resistant to docetaxel after repeated treatment cycles, recapitulating the human disease. When they analyzed these tumors, they found that expression levels of FOXJ1 and other related genes were significantly higher in resistant tumors than in those still sensitive to the drug.
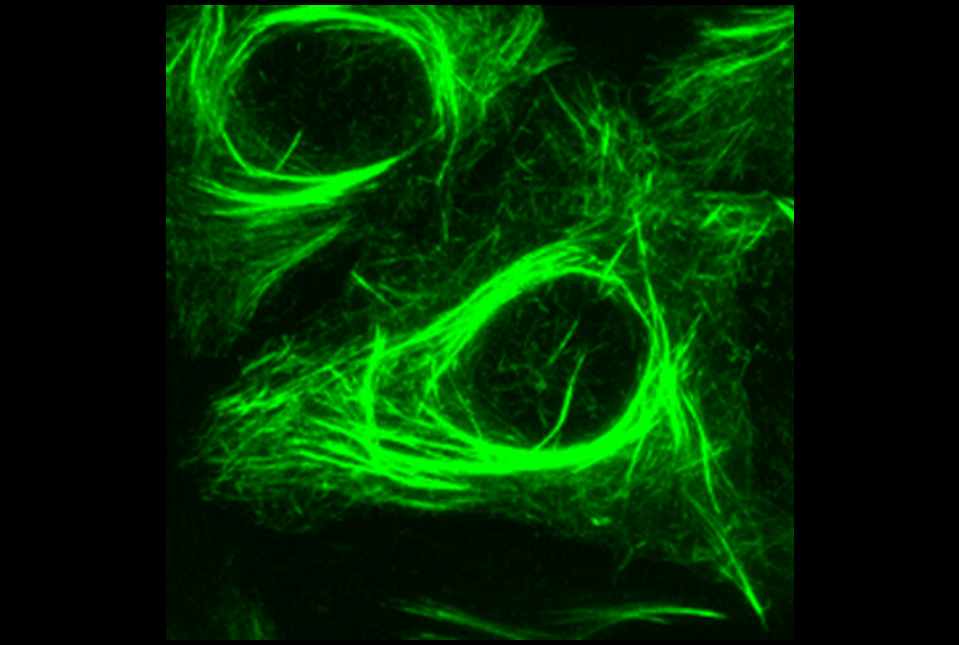
FOXJ1 is best known for controlling genes involved in the formation of cilia, hair-like structures extending from the cell surface. However, the researchers uncovered an unexpected role for FOXJ1 in regulating microtubules inside prostate cancer cells. Microtubules, dynamic structures that function as both scaffolding and transport tracks, are essential for cell division and survival.
Interestingly, taxanes, such as docetaxel, work by binding to microtubules, which stabilizes them and disrupts their normal dynamics. As a result, cancer cells cannot successfully divide and ultimately die.
When the researchers increased FOXJ1 levels in prostate cancer cells, the cells became less sensitive to docetaxel both in laboratory experiments and in patient-derived tumor mouse models. Conversely, reducing FOXJ1 expression made cancer cells more vulnerable to the drug.
“These findings are exciting as they identify a role for FOXJ1 in controlling microtubule dynamics in cells without cilia and show that tumor cells can exploit this function to develop resistance to taxanes,” said Dr. Steven Balk, professor of medicine at Harvard Medical School and oncologist at Beth Israel Deaconess Medical Center, who co-led this research.
The team went on to determine how FOXJ1 triggered drug resistance. They found that the drug’s impact was reduced when FOXJ1 activity altered the behavior of microtubules, which prevented docetaxel from binding and stabilizing them as effectively. The team also identified additional genes regulated by FOXJ1 that influence microtubule function, indicating that it orchestrates a broader network of microtubule-related genes that promote chemotherapy resistance.
Patient Data Aligns with Lab Findings
Beyond the laboratory, the researchers analyzed tumor samples from clinical studies. They found that FOXJ1 gene amplification was more common in patients who had been treated with taxanes. In addition, data from a large clinical trial indicated that patients whose tumors had high FOXJ1 levels before treatment had poorer outcomes when docetaxel was added to standard hormone therapy.
“It was clear that the patients who overexpressed FOXJ1 did not benefit as much from taxane therapy,” said Dr. Giannakakou.
Though further research is needed, the findings suggest that some tumors may already carry high levels of FOXJ1 before treatment, making them less responsive to chemotherapy. Exposure to the drug may also drive cancer cells to increase FOXJ1 activity as they evolve resistance.
“We are optimistic that these insights will allow us to improve taxane-based therapies in prostate cancer and other cancers where taxanes are used,” Dr. Balk said.



