
It is our mission at New York-Presbyterian Weill Cornell Medicine to train the next outstanding leaders in Maternal-Fetal Medicine (MFM). The MFM Fellowship Program provides fellows with extraordinary academic support in developing clinical excellence in high-risk obstetrics and promoting growth in all areas related to MFM through research, advocacy, and community involvement. With exposure to an unusually diverse patient population throughout New York City, fellows have a unique opportunity to study a range of clinical issues, often in collaboration with other departments to provide multidisciplinary care to patients. We aim to serve a broad population of pregnant patients and work to improve the lives of individuals and their families within our surrounding communities and around the globe.
Our active and renowned obstetrical ultrasound unit offers fellows the opportunity to train in all phases of non-invasive and invasive fetal sonography, while the antepartum testing unit offers the opportunity to develop skills in fetal assessment and provides a wealth of research opportunity. Additionally, the Alexandra Cohen Hospital for Women and Newborns is a state-of-the-art birthing facility with >8,500 deliveries per year, and its obstetric critical care units provide fellows many learning opportunities in inpatient high-risk obstetrics.
The Department of Obstetrics and Gynecology and the Division of Maternal-Fetal Medicine at Weill Cornell Medicine are recognized as leaders in clinical excellence as well as basic, translational, and clinical research.
Application Procedure
Fellowship applications are accepted via the Electronic Residency Application Service (ERAS). We welcome applications from candidates who bring a variety of experiences, perspectives, and identities to the table. New York State Medical License and Board eligibility for the American Board of Obstetrics and Gynecology (ABOG) are required for our fellows.
The minimum requirements for your application are:
- ERAS Application
- Personal Statement
- Letters of Recommendation – a minimum of 3 (ERAS can hold up to 4). We accept letters of recommendation in both traditional and SLOE formats.
- USMLE/COMLEX Scores
- Medical School Transcript
- Photo
We do not review CREOG scores in our assessment of applicants. Score reports are not necessary. Program signaling is encouraged.
Application Deadline
The application deadline for an August 2027 start date is April 27, 2026. Invitations to interview will be extended to selected candidates on May 18, 2026.
Virtual interview dates will be held on the following dates:
- Friday, July 10, 2026 (AM session)
- Friday, July 24, 2026 (PM session, non-East Coast candidates will be prioritized)
- Friday, August 7, 2026 (AM session)
Leadership

Moeun Son, MD, FACOG
Fellowship Director

Inna Landres, MD, FACOG
Associate Fellowship Director
Fellowship Coordinator

Zuzanna Smurzynska
Email: obgynmededucation@med.cornell.edu
Phone: (212) 746-3085
Salary and Benefits
At NewYork-Presbyterian Weill Cornell Medicine, we offer a comprehensive salary and benefits package to ensure our fellows are well taken care of while they train at our hospital. For more details, please visit NYP Graduate Medical Education to learn more about our current rates.
Housing
Modern luxury apartments in doorman buildings located within a block of the Medical Center are available to House Staff. Most of our Fellows take advantage of hospital housing because of its convenience to the medical center. There are three existing residential buildings: Helmsley, Payson, and Coleman. There are additional pre-war properties in the neighborhood.
For more details, please visit the NewYork-Presbyterian Real Estate website.
Meet our MFM Faculty

Current MFM Fellows

Anna Staniczenko, MD
PGY-7

Priyanka Gaur, MD, MPH
PGY-6

Rachel Friedlander, MD
PGY-5
Fellowship Program Highlights
- Active involvement in the multidisciplinary care provided by the Placenta Accreta Program and Obstetric Cardiology Program.
- Active involvement in the Fetal Care Center including participation in advanced needle procedures and complex deliveries such as EXIT procedures.
- Fellows serve as preceptors in the fellow-run outpatient high-risk clinic and deliver high-quality care to vulnerable patient populations with emphasis on resident education.
- Fellows help supervise and consult on busy inpatient services including labor and delivery, critical care, and the antepartum service.
- Strong program support for academic endeavors such as pursuing advanced research certificates, Editorial fellowships, CDC fellowship, and participating on committees for ACOG and SMFM.
- Outstanding clinical and academic mentorship opportunities from many mentors in MFM, research faculty, two triple-boarded MFM-Critical Care faculty, and dedicated teaching sonographers.
- Frequent collaboration with multiple specialties within Weill Cornell Medicine and with neighboring institutions including Hospital for Special Surgery, Memorial Sloane Kettering, and Rockefeller University.
MFM Research

Recent Fellow Presentations and Publications
- Staniczenko AP, Khander A, Landres IV. Delivery Planning in the Setting of Atrial Tachycardia and Heart Failure. Oral Presentation at The 9th International Congress on Cardiac Problems in Pregnancy. April 24-27, 2025. Vienna, Austria.
- Staniczenko AP, Darveau SC, Chasen ST. Obstetric outcomes in pregnancies complicated by placental mesenchymal dysplasia. Oral presentation at 2025 AIUM Annual Convention. March 29-April 1, 2025. Orlando, Florida.
- Staniczenko AP, Heaps S, Gasi L, Chasen ST, Scholl J. Prenatal diagnosis of cloacal exstrophy after referral for gastroschisis. Oral presentation at 2025 AIUM Annual Convention. March 29-April 1, 2025. Orlando, Florida.
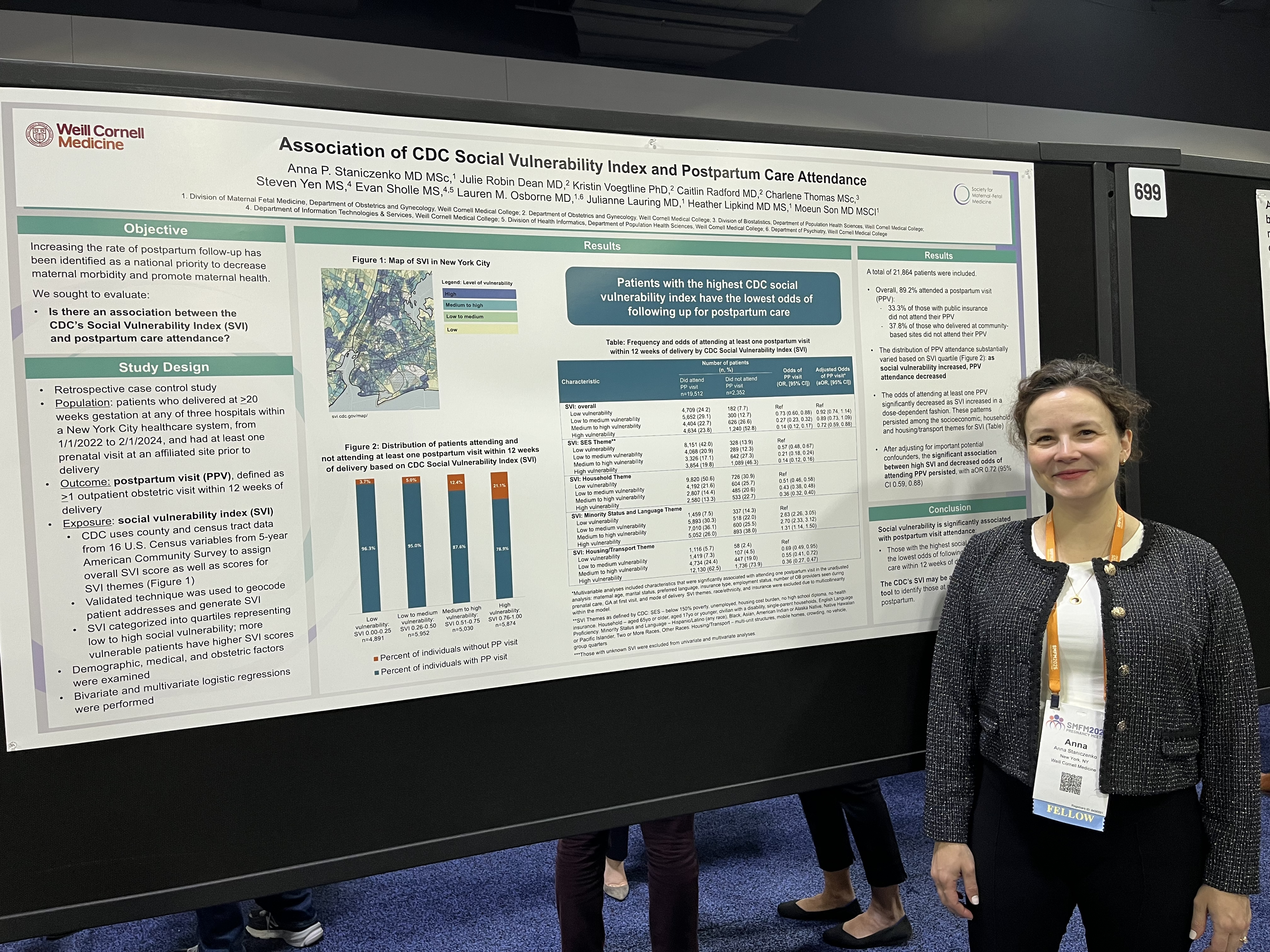
- Staniczenko AP, Dean JR, Voegtline K, Radford C, Thomas C, Yen S, Sholle E, Osborne LM, Lauring J, Lipkind H, Son M. Association of CDC Social Vulnerability Index and Postpartum Care Attendance. Poster presentation at Society for Maternal Fetal Medicine 45th Annual Pregnancy Meeting. January 27-February 1, 2025. Denver, CO.
- Staniczenko AP, Pudwell J, Ackerman-Banks C, Smith GN, Lipkind HS. Progression in AHA stage of hypertension and cardiovascular disease risk among ACOG-defined normotensive individuals. Poster presentation at Society for Maternal Fetal Medicine 44th Annual Pregnancy Meeting. February 10-14, 2024. National Harbor, MD.
- Society for Maternal-Fetal Medicine (SMFM), Gaur P, Goulding AN, Spong CY, Werner EF; SMFM Health Policy and Advocacy Committee. Society for Maternal-Fetal Special Statement: Transforming the maternity care team model. Pregnancy (Hoboken). 2025;1(3):e70018. doi:10.1002/pmf2.70018
- Gaur P, Darwin KC, Kohn JR, Uribe KA, Shippey E, Eke AC. The relationship between COVID-19 vaccination status in pregnancy and birthweight. Am J Obstet Gynecol MFM. 2023;5(9):101057. doi:10.1016/j.ajogmf.2023.101057
- Gaur P, Ganguly AP, Kuo M, et al. Childcare needs as a barrier to healthcare among women in a safety-net health system. BMC Public Health. 2024;24(1):1608. Published 2024 Jun 17. doi:10.1186/s12889-024-19125-1
- Friedlander R, Huang X, Zee P, et al. Sleepiness in pregnancy and adverse perinatal outcomes. Pregnancy. 2026;2:e70234. doi:10.1002/pmf2.70234
Life After Fellowship – Our Graduated Fellows




